Summary
The intervention
The Safer Births Bundle of Care is an evidence-based program that has been shown to reduce maternal and newborn deaths in low-resource settings. Developed as a result of more than 10 years of research, it includes innovative training and clinical tools and a focus on continuous quality improvement for scalability and sustainability over time. The program uses low-dose, high-frequency training for individuals and teams. Digital tools capture data for reflective debriefing, shifting the culture from “blame and shame” to continuous quality improvement.
The scale-up
This cost-effective program is now implemented in over 150 health facilities in Tanzania. The program trains and equips healthcare workers to manage the leading causes of newborn and maternal deaths, reaching over 280,000+ births annually, with plans for national expansion in 2025.
The evidence
Results from a large-scale study published in the New England Journal of Medicine show a 40% reduction in early newborn deaths and a remarkable 75% reduction in maternal deaths after implementation of the program in 30 hospitals in Tanzania.
Results
A proven lifesaving program
In February 2025, the New England Journal of Medicine published a large stepped-wedge cluster randomized controlled study from across the 5 regions with the highest maternal and newborn mortality in Tanzania.
The study showed a 40% reduction in early newborn deaths and a remarkable 75% reduction in maternal deaths after implementation of the Safer Births Bundle of Care program in 30 hospitals. The data was collected between March 2021 and December 2023, with approximately 300,000 mother-baby pairs recorded during the study period.
reduction in early newborn deaths
reduction maternal deaths
The research consortium
A wealth of new knowledge
Rigorous research sits at the heart of Safer Births. The Helping Babies Breathe study at Haydom Lutheran Hospital in 2010 was the first of over 150 published, peer-reviewed papers from the Safer Births Research Consortium. Whilst they didn’t know it at the time, what the researchers were beginning would become the largest newborn resuscitation research project in the world.
These 150 studies have contributed to a wealth of new knowledge that is improving outcomes for mothers and newborns globally.
Informed by 40 PhD studies
Rigorous research sits at the heart of Safer Births. So far, 150 peer-reviewed papers have been published as part of the project.

“What makes the program unique is that it is truly evidence-based, resulting from 10+ years of research and development. This is possible thanks to an active and dedicated group of researchers who collaborated with the government of Tanzania.”
Dr. Benjamin Kamala Principal Investigator, Safer Births Bundle of Care
Increasing impact
Iterative development of a bundled approach
-
2009–2012
Building on Helping Babies Breathe
Helping Babies Breathe and Helping Mothers Survive studies initiated by Haydom Hospital show the importance of low-dose high-frequency training.
-
2013
Safer Births is born
Data captured for every birth, establishing a culture for quality improvement and development of more efficient data collection tools.
-
2013–2016
New research informs best practice
Research evidence showed timely bag-mask ventilation, fetal heart rate monitoring, and on-site refresher training improved patient outcomes.
-
2013–2016
Clinical and training innovations developed
Validated by research, clinical and training tools are developed and tested to support healthcare workers improving care for mothers and newborns.
-
2017–2019
Focus on quality training
Well-trained local champions motivate regular skills training, whilst simulation facilitators – trained in an accredited course – deliver effective team trainings and drive quality improvement.
-
2019
A bundled approach
Safer Births Bundle of Care established as a four-part, comprehensive approach to reduce newborn and maternal deaths.
-
2020
Innovation-to-Scale award
Rated #1 out of 320 proposals by the Global Financing Facility, a trust fund hosted at the World Bank, the Safer Births Bundle of Care received USD 4.5 million in funding.
-
2021–2023
Safer Births Bundle of Care scaled
Implemented in 30 hospitals in Tanzania, preliminary results garnered additional funding of USD 8.5 million to scale-up to 150+ facilities in 2023.
-
2025
Launching in Nigeria
Safer Births Bundle of Care kicked-off in Gombe and Borno states to address high maternal and newborn mortality.
-
2025
Results published in the New England Journal of Medicine
Study showed reductions of 40% in early newborn deaths and 75% in maternal deaths after implementation in Tanzania.
The bundle
An impactful, long-term approach
The Safer Births Bundle of Care program is a health system strengthening approach. It focuses on developing the health workforce, data-driven quality improvement initiatives, alongside improved access to clinical and training innovations which target the leading causes of perinatal mortality.

Training innovations
Allowing for on-site, regular simulation training, using the Helping Mothers and Babies Survive educational materials, bridging the gap between knowledge and lifesaving skills.



Clinical innovations
Specially designed clinical innovations for use in low-resource settings, to support birth attendants to provide the best care for mothers and newborns.




Sustainability & scalability
Strong national and local ownership, adaptation to national guidelines, well-trained local facilitators, and regular mentorship together support the program’s long-term impact.
At least one person from each facility is trained in SimBegin (an accredited simulation facilitator course), supporting the delivery of high-quality, on-going team simulation training.

Continuous quality improvement
Collecting and analysing local training and clinical data to provide insights into knowledge and skills gaps, enabling birth attendants to reflect and improve.
LIFT is a digital tool designed to capture, store and analyze training data emerging from health facilities. The adoption of the tool allows for the program to be scaled.
Training innovations
Safer Births training innovations were designed in response to the need for improved clinical practice in managing birth related emergencies, especially in low-resource settings.
Supporting a culture of quality improvement
Situated in health facilities, these innovations are shown to motivate healthcare workers, increasing individual and team training, which improves provider competence and confidence.
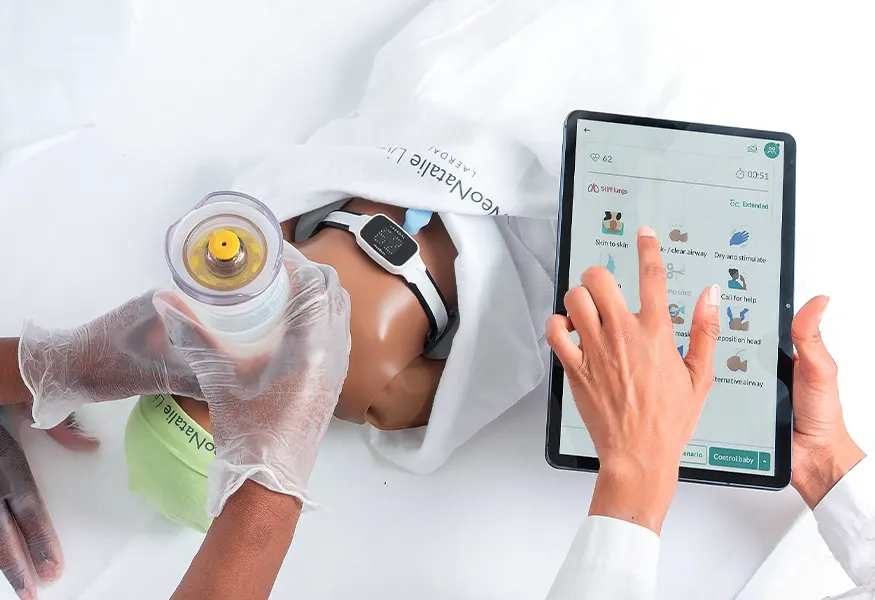
NeoNatalie Live
A smart manikin, providing immediate objective feedback on newborn resuscitation, simulating various lung compliance scenarios.
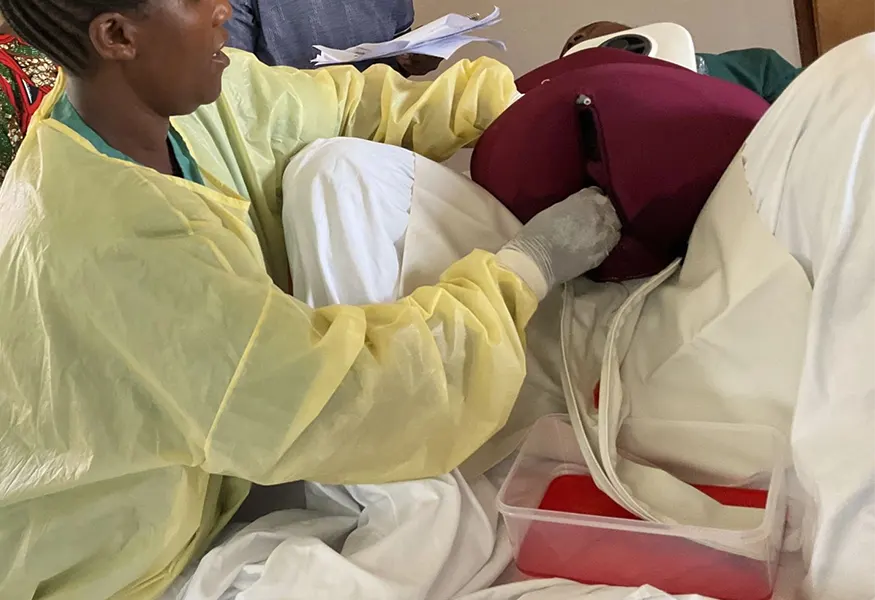
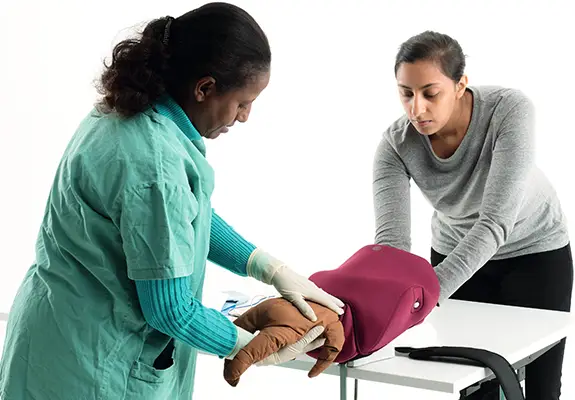
MamaNatalie
Supporting the globally recognized Helping Mothers Survive training programs, including the management of postpartum hemorrhage – the leading cause of maternal mortality.
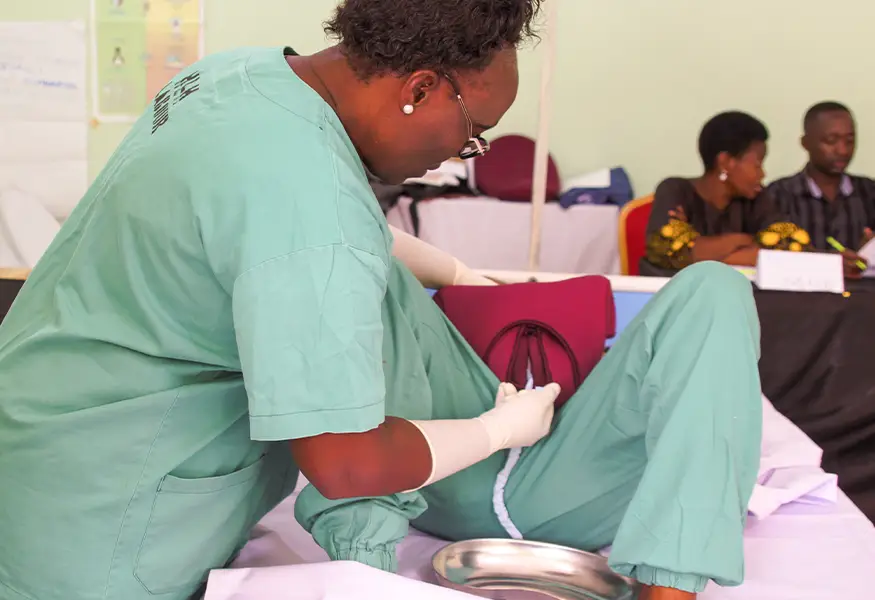
MamaBirthie
Designed to train for normal and complicated births, enabling healthcare providers to practice and improve teamwork and decision making using team simulation scenarios.
Clinical innovations
Safer Births clinical tools were developed to better support healthcare workers to make informed decisions and to provide quality care, in response to emergencies on the day of birth.
Replacing historical solutions
These clinical innovations replace ones that have been used for decades, some as long as 150 years. Each of these tools were validated through PhD studies, showing them to be more effective than the alternatives.

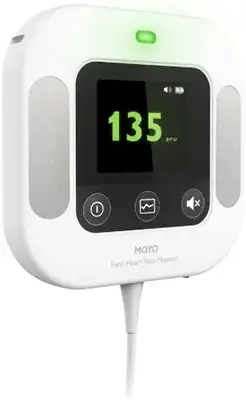
Moyo
A quick and accurate digital fetal heart rate monitor, used during labor to help healthcare providers make timely, informed decisions.
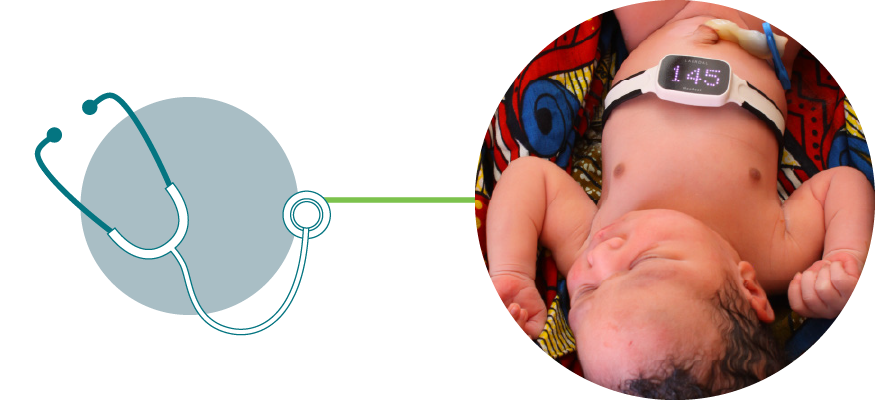
NeoBeat
A newborn heart rate meter, that takes seconds to put on a newborn’s torso, presenting the heart rate with an accurate digital display.
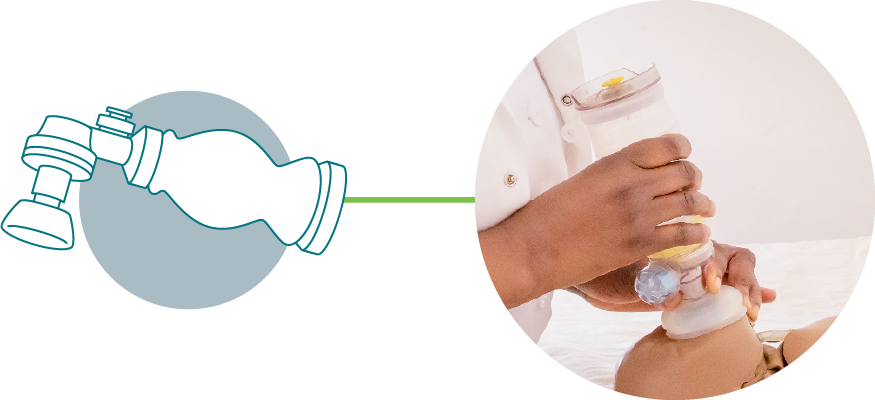
Upright Resuscitator
The innovative and ergonomic design and new face mask with better seal facilitates more effective positive pressure ventilation.
Penguin
A high-quality suction bulb designed to aid health workers to safely remove obstructing fluids from a newborn’s nose and mouth, to help them breathe.
Sustainability & scalability
Ensuring the impact of the Safer Births program is sustainable over time, including maintenance of competence, is central to the success of the program.
Government and local ownership
Safer Births Bundle of Care started in one hospital in Tanzania, then scaled to 30. It is now in over 150 health facilities, covering all CEmONC hospitals in 5 regions. Collaboration with the national health authorities (Ministry of Health and President’s Office, Regional Administration and Local Government Tanzania) has been central to the successful implementation of the Safer Births Bundle of Care in Tanzania.Trained simulation facilitators
To ensure that the program continues to be implemented, 2–3 facilitators at each facility are trained using the SimBegin program: a course giving the skills and confidence to plan, conduct and debrief a team simulation scenario. In one study*, healthcare workers expressed improved confidence and competence in managing the leading causes of maternal and newborn mortality. This was attributed to frequent facilitator-led team simulations with reflective debriefing.Mentorship
Strong mentors empower healthcare workers through supported hands-on training to refine clinical skills and by encouraging a no-blame culture. Mentors role-model best practices, provide learning opportunities, track progress over time, and deliver effective feedback and coaching.“The weekly team trainings have changed how we work together as a team. After every simulation training we sit down and discuss how we can improve.”
Ghai Abuya Midwife, Tabora Regional Hospital
Continuous quality improvement
Through the development of the Safer Births Bundle of Care lessons have been learned about what is needed to make simulation training translate into improved clinical practice, and better outcomes for mothers and newborns.
Weekly low-dose, high-frequency training
As part of the Safer Births Bundle of Care program, Skills Corners are established on-site within health facilities, allowing birth attendants to train regularly. Training innovations have been gamified to make the experience highly motivating for the healthcare workers.
Data-driven quality improvement
Data from simulation sessions is collected real-time and on an ongoing basis to support and guide facilitators on how to run quality simulations and enable more effective mentorship. Digital tools like LIFT capture training data and provide guidance for individual and group sessions, providing insights into training activities at regional, facility, or individual levels, to inform quality improvement discussions.
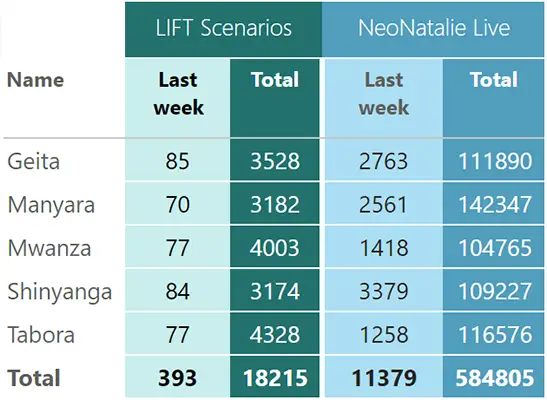
Program success factors
Five key lessons learned about what it takes to make the program work.
-
Local ownership
Engaging local stakeholders and national government from early planning to ensure ownership is taken throughout implementation – and that commitment sustains beyond implementation.
-
Local well-trained facilitators and champions
Empowered local facilitators can drive vital in-situ, team simulations. They — along with local champions — can also ensure the positive culture change that allows for continuous quality improvement.
-
Data-driven continuous quality improvement
Always guided by the local training and clinical data, regular training sessions target skills and knowledge gaps.
-
Ongoing mentorship and supportive supervision
Strong mentorship focussed on developing skills, uplifting confidence, supporting continuous improvement, role modelling best practices and fostering a peer-learning culture with consistent support.
-
Strong systems for equipment maintenance and reprocessing
Accessible user information for all who encounter equipment, alongside maintenance schedules and clear processes for reporting equipment issues.

Partnering to scale-up innovation
In 2019, the Global Financing Facility (GFF) partnered with Norad, UNICEF and Laerdal for an innovation-to-scale initiative to scale-up and test promising innovations with high impact potential.
Out of 320 proposals, Safer Births Bundle of Care was rated to have the highest impact potential, and received funding from the GFF.
The program continued to show remarkable impact and cost-efficiency and received a further USD 8.5m in 2023 for the scale up to 150+ health facilities. The program is set for national expansion in Tanzania, and beyond to other countries facing high levels of maternal and newborn mortality.

“Safer Births Bundle of Care in Tanzania shows the transformative advances that can be made to crash maternal and neonatal mortality if such highly cost-effective, and relatively simple innovations are taken to scale.”
Luc Laviolette Head of the GFF Secretariat

“Historically, many programs see quality drop after implementation ends. However, this program shows sustained improvements by strengthening healthcare workers’ capacity and fostering a positive culture change.”
Dr. Paschal Mdoe Executive Director, Haydom Lutheran Hospital
Guiding the way forward
The Safer Births Bundle of Care scaled from a single hospital to 30, and then to 150+ health facilities across Tanzania. Work is underway towards national scale up, which would see thousands more mothers and newborns benefit from better quality care on the day of birth.
Expanding into other countries
The success of the program has not gone unnoticed, with Nigeria already beginning its first implementation of the program in two states, Borno and Gombe. Ethiopia has also shown strong interest in incorporating the program into its national plans for reducing maternal and newborn mortality.
Cost-effective
Preliminary findings from an ongoing cost-effectiveness study are showing that the investment per life year gained is significantly below the World Health Organization’s threshold for cost-effective health interventions.
Continuing to invest in global health
Innovative funding models are critical for addressing maternal and newborn mortality on a global scale. These models enable the mobilization of resources necessary to implement successful health interventions, like the Safer Births Bundle of Care, and to ensure it is sustainable over time. By exploring models like public-private partnerships, government financing, and other innovative funding mechanisms we can create the supportive ecosystem necessary to drive lasting change. Together, public-private partnerships and the Global Financing Facility contribute to a world where more mothers and babies survive, leading to a better world for everyone, everywhere.

“I am proud that Tanzania was the first country to adopt and scale up the Safer Births Bundle of Care – and we are seeing the results. Thousands of lives are being saved, annually.”
Jenista Mhagama (Mb) Minister of Health, Tanzania